Let me ask you Doc?
The Importance of Baby Teeth
- by Dr Tony Widmonte BDS(Wits)

There are a lot of Moms and Dads out there who were unfortunately never taught by their parents the importance of baby or as we dentists call them “deciduous” teeth. So when their children get teeth its an attitude of: “ What’s all the fuss about baby teeth – they’re going to fall out anyway, so if they have holes what does it matter, the big teeth will soon grow.”
Thankfully that kind of thinking is not so common these days but there are still those who think that way.
Just stop for a moment and consider this: Why are healthy baby teeth so important? Why are we told that regular trips to the dentist are necessary twice or three times a year, even if your child doesn’t complain about his teeth. If a child doesn’t have pain or discomfort parents often wrongly believe that there is nothing wrong.
This is far from the truth. A child’s mouth may have several small or medium sized holes or cavities that are not yet large enough to cause pain – that’s why regular visits are recommended.
Baby teeth serve many significant functions which make it so important to keep these teeth healthy and free of decay.
- Eating, Speaking and Appearance
The most important reason for having healthy teeth is to enable the child to chew food into smaller pieces making digestion easier.
Initially infants are breast or bottle fed and the first solid food is soft mushy stuff because baby does not yet have teeth to chew with. By the child’s first birthday all the upper and lower front incisors have erupted. These teeth must be checked and adequately cleaned by the caregiver who should also ensure that the child eats healthy food.
A common pattern of early decay results from inappropriate bottle-feeding.
Desperate parents will often try to pacify a baby with a bottle of juice or other sweetened drink.
Unfortunately this leads to what is called ‘Baby bottle mouth syndrome’,
where the upper front teeth rapidly decay and if not treated end up as blackened unsightly stumps.
The child is burdened with these until the ages of 6 to 8 when adult teeth usually start to erupt.
This can have a devastating psychological effect on a child.
These front teeth are only swapped for adult teeth between the ages of six and eight. Imagine your child at nursery school with ugly, black teeth and with a speech problem. Without front teeth a child will develop a lisp because certain letters can only be pronounced with the tongue touching on the upper front teeth.
The teasing and ridicule by other children is very real problem and can result in an embarrassed, unconfident and withdrawn child, with a speech defect, who can remain like that into adulthood.
So correct bottle nursing, cleaning of teeth and the correct diet can be vital for the child who will one day be an adult.
- Losing baby/decidious teeth can cause problems for the jawbones, muscles and permanent teeth.
How can this happen?
You see, decidious teeth actually encourage normal development of the jawbones and muscles.
When a child chews, the pressure on the teeth encourages bone growth around the roots.
The muscles that open and close the bottom jaw are joined to the upper jaw as well. Here also during chewing and talking the muscles continually pull and put pressure on the bones and encourage normal growth.
Decidious teeth are designed to fit into a small jaw. As the jaw grows, the small teeth no longer fit the growing jaw, so we lose these teeth for larger adult ones.
However if a decidious back tooth is extracted due to decay, the tooth next to it may tilt or drift into the now empty space. In addition, the teeth in the other jaw may move up or down to fill the space left by the missing tooth.
When adjacent teeth shift or move up or down into an empty space left by a lost tooth, the space becomes smaller than it originally was, so a lack of space is created in that jaw for the permanent teeth to grow into.
So we often find that when the permanent teeth erupt they are crowded or cramped together in a smaller space and they may also come out rotated or in the wrong place or even remain permanently buried beneath the gum.
If left untreated, expensive and extensive orthodontic treatment may be needed to make the smile acceptable and give the child a confidant self image.
So you see Moms, Dads and Caregivers, teeth play an important role in how a child interacts with the world we live in – Please don’t forget that !!
Dental Hypnosis and Children
- by Dr Tony Widmonte BDS(Wits)

Hypnosis in dentistry is not widely used today but in the hands of a trained and experienced Dentist or Hypnotherapist its advantages can be quite profound.
Children usually make excellent hypnotic subjects.
They have such wonderful imaginations that you can easily induce a hypnotic state by persuading them to imagine taking off in a spaceship or taking part in their favourite television show by allowing their eyes to be the television sets.
A large percentage of childhood and adolescent problems stem from unresolved emotional issues. These children are often anxiety ridden with a lack of confidence and they become totally dependent on one or both of the parents. They sometimes exhibit various problems such as nail biting, stuttering, obsessive compulsive disorders, bed wetting, behavioural problems, nightmares and even bulimia. Hypnosis can resolve some of these symptoms but in others individual and family therapy is necessary.
From a dental aspect the thumb sucking, grinding, examination anxiety and bulimia (in the older children) are the main problems. The child with examination and treatment anxiety is the most difficult to treat as they are usually very young children and communication is difficult. Some cases will certainly respond to hypnosis while others can only be treated with tranquilisers or general anaesthetics.
When you take your child for a dental examination you as the parent will know if your child is going to be difficult to treat or not. Under such circumstances be honest with yourself and don’t be embarrassed - there are lots of nervous children - discuss with your dentist the different options available for treating your child.
Remember it is vital that your dentist is sympathetic to a fearful child because if he is mishandled you may land up with a patient who is terrified of the dentist for the rest of his/her life.
If you think your child might respond well to hypnosis then ask your dentist and if he thinks this a viable alternative then he can refer you to someone - but if he is prepared to treat your child and doesn't think it such a good idea then you should be guided by him - after all, he is your dentist.
Thumb-Sucking and Tips on Breaking This Habit, Eventually
- by Dr. Sameera Yusufmia

It’s always wonderful to watch adoring parents gaze with pride at their newly-born sucking his/her thumb. This self soothing habit gives intense joy to the little ones and us as dentists have recognised and accepted this, hands down!
Sadly though, this cute picture can get quite complicated and ugly when the child continues this habit over the age of four and for some until the age of twenty! In this case we and the majority of society frown upon this.
Thumb sucking is definitely an inborn natural habit that a child uses to comfort him/herself when he/she is:
*Anxious
*Stressed
*Bored
*Unhappy
*Hungry
Some children may develop the habit later when they try and imitate a younger sibling.
As a parent, you need to know:
*When you need to be concerned
*If and when your child needs intervention (either by you or a health professional).
Background facts that you need to consider include:
*About 70% of all children thumb-suck from infancy and naturally grow out of it by the age of four.
*Only about 10% of these continue with the habit after the age of four
*The harmful effects of thumb-sucking are dependent on its duration, frequency and intensity.
Harmful effects that you need to be aware of include:
*Deformities-oddly shaped fingers or thumbs
*Infections-due to the constant moistened areas the skin gets irritated and infected
*Social –The child may be made fun of at school and socially.
*Dental and Facial- the intense negative pressure that is created in the mouth affects the facial muscles, the teeth and the jaws. The upper jaw becomes more ‘V’ shaped. The upper front teeth flare outward. The lower front teeth tip inward. This results in a child having an ‘open bite’. This is when their anterior upper and lower teeth don’t meet when they bite. This in turn affects their speech, chewing, swallowing and facial appearance.
Coping with your child’s habit
* Let your dentist assess your child at an early age. You will be advised of any noticeable problems if any and subsequently on when you need to try and assist in discontinuing the habit.
* In the case where the child shows very little effect in the mouth, the parent still needs to consider the negative social aspect and try and intervene at least by the age of five.
Studies have shown that most children want to stop by the age of six. They just need to be guided. Your role is to guide them without any pressure. To be firm but calm and to support and praise them every step of the way.
Many suggestions to break the habit have been made and we hope these tips can help you! These are advised for children over four years, as the child must be able to comprehend and show some readiness.
Tip 1. Make your child aware of the habit and understand the ill effects.
The habit may be an unconscious one and you need to identify it with your child. Calmly point out to the child what you don’t like about the behaviour and why. Show them what their fingers /thumb looks like. Point out any calices Simple explanations may help. Talk about ‘bad’ germs that live on their fingers and that go into their mouths and make them sick. You could exaggerate a little, if it helps!
Tip 2.Keep tract of when your child is sucking his/her thumb.
Observe and identify when and how often your child sucks his/her thumb. It allows you to ascertain how deeply entrenched the problem is. If it happens at bedtime, or while the child is watching television, instead of socially then it is considered as a less serious problem. If it is clear that the child is doing it as a direct result of a stressful situation, then you first may have to deal with the child’s emotional well being before trying to stop the habit.
Tip 3.Distraction, keeping hands busy.
By identifying the exact times that the child may thumb-suck, allows the mum to quickly intervene by offering the child something to occupy their hands with. Finger puppets have shown to assist in occupying little hands. Promote activities that use both hands such as doing a puzzle or playing with a ball. (Instead of watching TV with idle hands).If it is a bedtime habit offer the child a soft ball to squeeze instead. Tell the child if they squeeze and hold on to the ball all night it will magically turn into another toy in the morning. You need to then obviously replace the ball with a little treat each day!
Tip 4.Creating a reward system
Breaking the habit is much easier when the child is a willing participant. Make a progress chart with the child; let him or her choose the stickers. Set an attainable target specifying the number of days. The child can then be given a star for each day that he or she doesn’t thumb-suck. When the target has been reached a desired reward is earned. To permanently end the habit a chart for few months is recommended. Daily praise for each star earned is paramount. In addition discuss with the child, how many slip-ups he is allowed and stick to that.
Tip 5 Controlling temptation
Many deterrents have been used and are available and have worked with some success especially in older children. Topical bitter substances, bandages, glove-like devices are normally used and worn on the offending finger.
Tip 6.Scheduled thumb sucking-partner in crime
This is a controversial suggestion, but has shown some positive results. A pact is made with the child. The child is asked to engage in the habit only at a specific time for a certain time daily. This is aimed at making the habit obligatory instead of involuntary resulting in it becoming less appealing to the child!
Tip 7.Dental appliance
If you have been unsuccessful with the above stated tips, don’t despair, there is a last resort. The greatest benefit of this is that it stops the habit in its tracks. It involves placing a fixed appliance in the child’s mouth (over the age of 6).It has a ‘gate’ or ‘crib’ like wire that lies behind the upper front teeth and prevents the thumb from getting to touch the palate .
Before choosing this intervention the child and parent must be educated and prepared.
Due to the immediate halting of the habit, the following problems may be expected:
*unhappy, irritable child
*few restless nights
*irritation and infection on palate caused by the appliance in the mouth.
In most cases the benefits have outweighed the risks. The child has normally continued treatment with more appliances to correct any other problems caused by the habit.
Finally one must understand that a habit takes time to develop and thus, it will also take time to be replaced by an alternative. As a parent be patient, consistent and focused on helping your child. Seek constant guidance and support if necessary.
Are You Feeding Your Kids Tooth-Friendly Foods
- by Dr Marietjie WeakleyBChD(Pret) dipOdont(UWC)

Are you feeding your kids tooth-friendly foods
As parents we all try to get our children to eat snacks and lunches that are good for their growing bodies and teeth. This can be a daunting task – with their friends eating sugary and starchy junk food! Advertising in the media, food sold in grocery stores and peer pressure, provides a big challenge for parents to make healthy food choices for their children.
Q: What is a healthy diet for my child then?
A balanced diet will supply all the nutrients your child needs to grow. If they lack certain nutrients, the development of healthy, decay-resistant teeth and gums, will not be possible. They need enough raw fruit, vegetables, grains, meat, beans, nuts, cheese and milk.
Q: How does children’s diet affect their dental health?
Increased, regular intake of starches and sugars will increase the risk of tooth decay. The added sugars in refined food and soft drinks assist plaque to develop and accumulate on teeth.
Q: How does plaque formation cause tooth decay?
Plaque is a sticky layer full of bacteria on teeth. These bacteria digest some of the sugars and produces acids that can weaken tooth enamel. If the acid remains on the tooth surface for a long time, it can cause those areas of the tooth to decay.
Q: Which foods are bad for the teeth?
Some foods and drinks have a high sugar and acid content. This includes: sweets, chocolates, cookies, cake, sugar-containing cool drinks (especially fizzy drinks!), snacks that stick to teeth, some cereals, chips, crackers and dried fruits.
The harder and tougher food, the worse the effect on the teeth will be. Marshmallows and jelly-type of sweets could be chosen instead of hard suckers and toffees!
Q: Are all sugars harmful to teeth?
Natural sugars in milk and fruit are not regarded as a significant problem. The added sugars in foods and drinks are a risk not only to the teeth, but also to general health!
Q: Is there any replacement for cane sugar?
A healthy alternative that reduces 80 % of tooth decay is Xylitol. This can be used as a sugar replacement. It is also recommended to use Xylitol on a daily basis, for instance in the form of sweets, sugar-free Xylitol containing chewing gum, Xylitol gel, etc.
Q: How do I establish healthy eating habits?
- It is easier to do this when children are very young and parents are more or less in control of their diet.
- The volume of sugar consumed is important, but it is the frequency of sugar and starch intake that does the most damage.
- Offer your children fruit instead of sweets or chocolates.
- Teach them to “dilute” the acidity in the mouth regularly by regular intake of water after meals and in between snacking.
- Eating cheese after a meal can reduce the effect of acid in the mouth.
- Babies should not be put to bed and left with a bottle of juice or even milk, as this can cause baby bottle decay. Plain water is the safest drink for the baby between feeding.
Q: Is there any other foods that can help prevent tooth decay?
- YES! Certainly! Foods that require vigorous chewing such as raw fruit and vegetables stimulate the flow of saliva. Saliva dilutes acids and helps to wash food away.
- Older children can chew sugarless Xylitol-containing gum that will also stimulate saliva production.
-
TIPS:
- Keep only nutritious foods in the house!
- Restrict high-sugar foods to set mealtimes rather that giving it by itself as a snack.
- Serve cheese as part of lunch or a snack
Q: What about fruit juices, sports drinks and flavored milk?
Unfortunately fruit juices contain very concentrated fruit sugars, which could be really damaging to teeth, especially given in bottles or sippy cups. This would feed bacteria that produce acids and attack the teeth.
Sport drinks and flavored milk also contain huge amounts of sugar and continuous sipping on this could cause severe tooth decay.
Q: What about birthday parties!!!?
Let children brush their teeth before they go to a birthday party. This would clean the mouth of plaque, and dilute acids, and prepare the mouth for the “acid-attack” at the birthday party!!!
Teach them to drink as much water as possible after having sweets, snacks or sugar containing drinks.
REMEMBER:
- A HEALTHY DIET IS NOT ONLY GOOD FOR DEVELOPMENT OF TEETH, BONES AND BODY. IT ALSO ADDS TO BUILDING UP THE RESISTANCE AGAINST VIRAL AND BACTERIAL INFECTIONS.
- OUR BRAIN NEEDS NUTRIENTS AND ENOUGH WATER TO BE ABLE TO THINK, LEARN AND REMEMBER.
- A NUTRISIOUS DIET PRODUCES ENOUGH ENERGY TO GET US THROUGH THE DAY!
- A HEALTHY BODY KEEPS A HEALTHY MIND!!!
- EXCERSIZE REGULARLY
- GOOD LUCK IN ENCOURAGING YOUR CHILDREN TO EAT GOOD, HEALTHY, FOODS. AND SEEING THAT ROME WAS NOT BUILD IN ONE DAY – BE PATIENT AND PERSERVERE! IT IS DEFINITELY WORTH IT!!!!
Xylitol - The Sweet Truth
- by Dr Janet Gritzman
BA, BDS(Wits), P.D.D.(PTA)Dip Odont Endo(PTA), Dipl.Dent (Conscious Sedation & Pain Control)(UWC).
President of Paedodontic Society of South Africa

Most children have a sweet tooth. They prefer to eat sweets rather than any other healthy alternative.
While artificial sweeteners are sometimes recommended to help keep kids away from sugar, not every parent is happy with the idea of chemically-produced sweeteners.
Now there's a natural sugar substitute that, not only does not cause cavities, it actually prevents them!
Xylitol is "tooth-friendly," a naturally occurring, low-calorie sugar substitute with
anticariogenic properties.
Xylitol is 5-carbon sugar alcohol.
Xylitol is produced in small amounts in the human body- as part of our normal metabolism, the body produces up to 14 grams in the liver daily.
It is found in many fruits and vegetables such as plums, corn and strawberries. The main source of commercially produced xylitol are corn cobs and birch bark.
Properties
It equals the sweetness of sugar and it has no after taste
It has 40% fewer calories than sugar. One teaspoon (5 gm) of xylitol contains 9.6 calories, as compared to one teaspoon of sugar, has a which has 15 calories.
It has a very low glycemic index of 13 (glucose has a GI of 100).
Its metabolism does not require insulin.
Xylitol-based products are allowed by the U.S. Food and Drug Administration to make the medical claim that they do not promote dental cavities.
It is approved in over 35 countries
How it works
The Streptococcus mutans bacteria is the main cause of tooth decay .
1. This bacteria uses sugar alcohols, sugars and other carbohydrates for food through fermentation.
In doing so, it produces acids that eat through the enamel on the teeth, which leads to decay. Streptococcus mutans cannot ferment xylitol- so in fact xylitol starves the bacteria.
2. Xylitol causes the environment to become more alkaline, inhibiting the bacterium’s growth.
3. Xylitol causes bacteria to lose the ability to adhere to the tooth, stunting the cavity causing process!
4. In addition xylitol accumulates intracellularly in Strep. Mutans, and this accumulation inhibits the bacteria’s growth.
The safety factor
Various committees and advisory boards have reviewed the safety data for xylitol. They have found no health concerns or placed any limits on consumption. The only side effect is when xylitol is taken at doses exceeding 20 to 40 grams or more. This may cause diarrhoea,in some cases.
Short-term consumption of xylitol is associated with decreased Streptococcus mutans levels in saliva and plaque.
Xylitol is safe for pregnant and nursing women.
Studies show that regular use of xylitol by nursing mothers significantly reduces the probability of transmitting the Streptococcus mutans bacteria, (which is responsible for tooth decay), from mother to child during the first two years of life, by as much as 80%. Researchers in Finland reported six-year results of a study that showed that mothers who chew gum sweetened with xylitol are less likely to transmit cavity-causing bacteria to their children.
Xylitol Products
Food products containing xylitol, including chewing gums and mints, are available commercially
There is no scientific evidence available to establish the value of xylitol-containing nasal sprays or xylitol sweetened children’s vitamins in preventing dental caries.
How to use it
About 6 g of xylitol per day is needed to counteract the production of acid and thereby reduce the risk of cavities.
The daily intake should be distributed over at least three occasions.
Xylitol products that actively stimulate the secretion of saliva should be the first choice, such as chewing gum. The increase in saliva buffers the acids in the mouth (acid is one of the major factors which cause demineralization of the teeth leading to decay) and helps to wash away food particles when you can't brush after a meal.
Chew 1.5-2 grams of xylitol gum for 5 minutes, 3-5 times a day.
It is best to chew xylitol gum after meals or snacks.
Xylitol sweetened mints can be used by people who can't or prefer not to chew gum.
Remember: xylitol candy and gum should not replace the need for regular oral hygiene. Even with the proper amounts of xylitol, brushing, flossing and regular dental visits are necessary to prevent tooth decay.
The Dental Check-up
- by Dr Janet Gritzman
BA, BDS(Wits), P.D.D.(PTA)Dip Odont Endo(PTA), Dipl.Dent (Conscious Sedation & Pain Control)(UWC).
President of Paedodontic Society of South Africa

At what age should a child have his/her first dental check-up?
Early visits to the dentist have been strongly recommended to help reduce the number of infants and children who suffer from preventable tooth decay.
Ideally we like to see children have their first dental check-up by their first birthday.
- Examining the child gives the dentist an opportunity to examine the mouth and confirm normal oral development.
- The dentist can check on the cleanliness of the mouth and teeth and for any signs of tooth decay. It gives the dentist an opportunity to give advice on prevention,
- It provides the parents with a chance to discuss oral hygiene practices, teething and mouth habits.
- Allows the child to become familiar with the dental environment. A non threatening, fun-filled first encounter with the dentist will encourage a positive attitude to dentists and future dental treatment.
How often should a child visit the dentist?
The Paedodontic society of S.A. recommends a 6 monthly dental check-up for most children. Some children will need more frequent dental visits because of increased risk of tooth decay, unusual growth patterns or poor oral hygiene.
Why should a child go to the dentist if he/she does not have toothache?
- Cleaning and polishing the teeth remove debris that build up on teeth, irritate gums and cause decay.
- Fluoride treatments strengthen teeth and prevent cavities.
- Oral hygiene instruction improve children’s brushing and flossing, leading to cleaner healthier teeth and gums.
- Regular dental check-ups, enable the dentist to locate caries early, and treat it before it causes pain and spreads to other teeth.
- Tooth decay isn't the only reason for a dental examination. The dentist will also assess changes in the child's oral health and identify orthodontic problems.
- If the dentist is adept in dealing with children, he/she can make the dental appointment fun and exciting. Regular dental check-ups will enable the child to become familiar with the dental surgery and eliminate the fear of dental appointments and dental treatment.
What happens at a dental check-up?
- The dentist will take the child's medical and dental history.
- He/she will do an examination of the child's teeth, oral tissues and jaws.
- The teeth will be cleaned and polished.
- An application of fluoride solution administered.
- The dental equipment will be introduced to the child in an interesting and non threatening manner so that the child will become familiar with the dental environment and comfortable with dental treatment.
- The dentist will also be able to talk to the child about the importance of caring for ones teeth in words, pictures and ideas in a way that the child can understand, so that he/she will be motivated to take responsibility for a healthy smile.
What steps can I take to ensure my child has good dental health?
- Eat healthily - avoid frequent snacking
- Brush properly twice a day
- Floss once a day
- Visit dentist regularly - 6 monthly
- Place fissure sealants on all permanent molars
- Ensure you child is getting the correct amount of fluoride
Fissure Sealant
- by Dr. Stephan Horwitz (BDS(Wits))

A fissure sealant is a resin which is placed in the grooves and fissures on the biting surfaces of molar and premolar teeth in order to form a protective barrier in areas where the end bristles of a toothbrush cannot reach.
Plaque and bacteria which accumulate in the grooves and fissures may eventually lead to tooth decay and thus fissure sealants are probably the most effective direct method of preventing tooth decay.
Sealants should be placed as soon as possible after the eruption of the permanent teeth at about six years of age.
It is essential to keep the tooth surface dry during placement of the sealant. The grooves of the tooth are prepared by the dentist or oral hygienist with a mild acid and then air dried.
The sealant is a resin in a flowable form which is carefully placed on the surface of the tooth and allowed to flow into the fissures. A curing light is then used to set ( harden ) the resin and the sealant is thus bonded onto the tooth and into the fissures.
Sealants can last for many years but may need to be periodically reapplied. Sealants afford protection to the fissures until the child is less prone to decay i.e.in late teens or early twenties.
The sealed surfaces are also smoother and more even making it easier to brush properly.
Dental sealants are an easy, quick, effective and painless way to help prevent tooth decay.
What Should I Do If My Child Has Toothache
- by Dr Janet Gritzman
BA, BDS(Wits), P.D.D.(PTA)Dip Odont Endo(PTA), Dipl.Dent (Conscious Sedation & Pain Control)(UWC).
President of Paedodontic Society of South Africa

- Rinse the mouth with warm salt water.
- Place a cold compress on the face if it is swollen.
- Give the child paracetamol (Panado) for pain.
- Do Not – place asprin on the teeth or gums.
- Visit the dentist as soon as possible
Oral Hygeine For Children
- by Dr Janet Gritzman
BA, BDS(Wits), P.D.D.(PTA)Dip Odont Endo(PTA), Dipl.Dent (Conscious Sedation & Pain Control)(UWC).
President of Paedodontic Society of South Africa

Why is it important to clean my baby's mouth and teeth?
Cleaning a baby’s mouth and teeth is important for the preservation of healthy teeth and gums, and maintaining the general health of the child. By instituting a teeth-cleaning routine into the child’s daily hygiene it sends a positive message to the child that caring for ones teeth is important.
How do I clean my baby’s mouth and teeth?
- From Birth till about 3 years:
At bath time a small clean gauze pad or dry wash cloth can be used. The teeth, gums and tongue are firmly wiped to remove liquid and food debris. Once the teeth have erupted the cloth can be dipped into a fluoride mouth rinse before wiping the teeth.
- From 3 - 6 years of age:
When the child is old enough to hold and manipulate a toothbrush, which generally occurs at about 3 years of age, the child can be given its own toothbrush with a miniscule amount of toothpaste and encouraged to brush his/her own teeth. There are a large variety of very good childrens' toothbrushes and toothpastes on the market. The size and shape of childrens' toothbrushes are especially designed for easy manipulation. They have small heads, soft bristles and can be easily gripped.
Please Note:
This should be in addition to the mother (care giver) cleaning the child’s teeth with a toothbrush or gauze and not instead of it.
The element of fun
One should aim to make teeth cleaning a fun, mother (care giver) / child bonding experience. If an activity is viewed by the child as enjoyable rather than a chore it will gain its own momentum. This is the best way to ensure that good oral hygiene practices are maintained for life.
Some ideas on how to do this:
When you are bushing your own teeth, put the child on the vanity slab of the bathroom and let him/her brush their teeth at the same time.

Children love to copy and participate in important activities.
A star chart and words of encouragement and praise go a long way to make oral hygiene fun and important in the child's mind.
-
From 6 years of age:
- Floss the teeth
- Brush teeth – using a pea size amount of toothpaste
- Massage the tongue gently
- Rinse with a teaspoon of mouth wash (containing fluoride) for about 20 seconds. This must be done under parental supervision to ensure the child does not swallow the mouth rinse. After using the mouth rinse the child should not eat, drink or rinse his mouth out with water for at least 20 minutes.
- This oral hygiene routine should be done under the watchful eye of the parent. The parent should evaluate how well the teeth were cleaned. If the child is not cleaning his teeth properly the parent should then clean the child’s teeth. A good way to monitor how effectively the teeth are cleaned is to use disclosing solution tablets after brushing. These can be purchased from ones dentist.
How often should children brush their teeth?
Children’s teeth should be cleaned twice a day. Ideally in the morning after breakfast, and at night before going to sleep. After brushing the teeth at night nothing should be eaten or drunk except water.
When should I start to floss my child’s teeth?
Once the teeth have erupted the mother (care giver) should floss the child’s teeth. As soon as the child has the manual dexterity the child should be encouraged to floss his/her own teeth. This generally occurs around 6 years of age. Again not instead of the mother flossing, but in addition.
Flossing, as well as being important for oral hygiene, is very good fine motor coordination training.
Mouthguards (Updated 2010)
- by Dr. Bradley Selvan (Private Practice)

- Dental injuries are the most common type of orofacial injury sustained during participation in sports; the majority of these dental injuries are preventable.
- A sportsman/woman is 60 times more likely to sustain damage to the teeth when not wearing a protective mouthguard.
- The cost of a fractured tooth is many times greater than the cost of a dentist diagnosed and designed professionally made mouthguard.
- Every athlete involved in contact sport has about a 10% chance per season of an orofacial injury, or a 33-56% chance during an athletic career.
- The cost to replant a tooth and the follow-up dental treatment is about R20 000-R50 000.
- Victims of tooth loss tooth who do not have a tooth properly preserved or replanted may face a lifetime of dental costs, hours in the dental chair, and the possible development of other dental problems such as periodontal disease.
- The stock mouthguard which is bought at sports stores without any individual fitting, provide only a low level of protection, if any. If the wearer is rendered unconscious, there is a risk that the mouthguard may lodge in the throat potentially causing an airway obstruction.
- Types of dental injuries (direct and Indirect) and intrinsic and extrinsic factors:
- Direct Trauma for example to the upper top front teeth (four times more common than other teeth) and the mouthguard must be well fitting and thick enough to prevent these injuries.
- Indirect Trauma for example under the chin causing damage to the teeth and concussion.
- Intrinsic Factors for example teeth position e.g. Class 2 or 3.
- Extrinsic Factors for example a hockey ball, fist etc.
- Classification of Mouthguards: From worst to best.
- Type 1. Stock (Small, Medium and Large)
- Type 2. Boil and Bite (Bought from stores and made from thermoplastic materials)
- Type 3. Custom, single layer, vacuum. (Types 3 and 4 supplied by the dentist)
- Type 4. A custom fabricated mouthguard formed on models of the users jaws, using multiple layers of plastic adapted under pressure to specific designs.
General design principles
- Mixed dentition- to distal of maxillary first molar.
- 2-3 mm labially
- 3 mm occlusally
- 2 mm palatally
- Labial flange 2mm from vestibular reflection
- Palatal flange 10 mm from gingival margin
- Even occlusal contact
For extreme sports the mouthguard should be extended to the distal of the second molars.
Mouthguards are made by pressure lamination at 140 C at 6 atmospheres of pressure with machines like a Drufomat or a Biostar.
Recommendations from Prof. Francois De Wet - Pretoria University
- Gr 1-5: 1 x 3 mm sheet
- Gr 6-9: 1 x 4 mm sheet
- Gr 10-12: 1 x 2 mm sheet with a 1 x 3 mm sheet over it
- Seniors: 1 x 2 mm sheet, then a layer of sponge, then a 1 x 3 mm sheet over everything
- Boxers: Same as seniors. Can increase the thicknesses even more.
Dr. Brett Dorney’s Recommendations (Australian Sports Dentist) for mouthguard designs
- Rookie (up to 14 years of old) 3mm +2mm (labial 3mm and occlusal 3mm)
- Classic (teenage years) 3mm+3mm (labial 3mm and occlussal 4mm)
- Elite 2mm+3mm+3mm with balanced occlussion distal of first molar ( labial 4mm and occlusal 4mm)
- Boxer 4mm+3mm extended over all the upper teeth with balanced occlussion (labial 5mm and occlusal 4mm)
I encourage my patients to have proper mouthguards made – one day your properly designed mouthgurad may save their life!
What Should I Do If A Child's Tooth Is Knocked Out
- by Dr. Bradley Selvan (Private Practice)

The incidence of dental trauma, to a child’s front teeth (usually upper teeth) has increased over the last few years, due to accidents, sport related injuries and violence. Protruded upper incisors and insufficient lip closure may be predisposing factors. Knocked out (avulsed) upper front permanent teeth, account for up to 16% of all traumatic injuries to permanent teeth.
Both primary and secondary teeth are vulnerable and can be “knocked” right out of the mouth. It is not always easy to tell the difference between primary and secondary teeth and all avulsed teeth, should be replaced into their sockets. The dentist will advise you, if it’s a primary or secondary tooth and whether or not it’s worth splinting and trying to save. Trauma can result in teeth being forced inward, upward, or downward from their sockets, or in a combination of these directions. While these injuries need urgent attention by your dentist, they don’t require immediate emergency treatment by you, the parent or responsible care giver.
Golden Rules for successful re-implantation.
- NB! Teeth knocked out of the mouth, need to be found and pushed back into their socket/s as soon as possible! The quicker the tooth is replaced the greater the chance of success. Best results are obtained, if the tooth is replaced in the socket, in less then 20 minutes. It is important to find the tooth to make sure that it hasn’t been swallowed or inhaled, into the bronchi or lungs.
- The tooth must be grasped firmly between your clean fingers (try not to touch the root surface) and pushed gently back into their socket/s.
- If it doesn’t look like it’s facing the right way around or doesn’t fit well into the socket, then turn it around and try again, or try another socket.
- If you are unable to replace the tooth or are too squeamish to try, then you will have to store the tooth in a clean container with the following liquids. Listed from best to worst: Hanks Balanced Salt Solution (biological medium) or milk which is found almost everywhere, sterile saline which may be difficult to find. The tooth can be stored in the child’s mouth, but care must be taken that the tooth isn’t swallowed or inhaled. This isn’t ideal as saliva is a septic medium. Tap water may be used as a last resort.
- The main aim is to replace the tooth quickly and cleanly so that there is minimal damage to the root cementum and periodontal (gum) tissues to try and prevent infection of the root canal.
- Get to your dentist immediately. They will check that the tooth is positioned correctly and using a flexible splint will stabilize the tooth for at least 7-10 days and probably even longer.
- The dentist will advise about the necessity of an anti- tetanus injection, mouth rinses and if necessary an antibiotic. A soft diet is recommended, with gentle tooth brushing after meals, with a soft brush.
- Wearing a custom made bite plate can save your child’s very valuable front teeth and smile. Bite plates can prevent fractures of the jaw and by preventing concussion, can save your child’s life! Ask your dentist about these mouth guards.
Does My Child Suffer From Bruxism
- by Dr Sameera Yusufmia (Bchd, Dip Clin Dent)

Bruxism is defined as the involuntary grinding of teeth especially at night. It results in wear of tooth surfaces due to tooth to tooth contact i.e. attrition.
How can I check?
You will either notice the noise created by the child grinding his teeth during sleep or you will actually see the physical “shortening” of certain teeth.
What is it caused by?
Many theories have been suggested and include
A) Psychological factors:
a) Stress- due to a new environment, a divorce, issues at school etc.
b) Overactive children-These children tend to burn off extra energy at night by grinding!
B) Inner ear:
This relates to the pressure that may build up. Children grind to try and equalize any pressure changes.
C) Disproportionate jaws:
The top and bottom teeth may not fit together comfortably.
D) Side effects of medication:
Children that may suffer from cerebral palsy may be on medication that contributes to grinding.
What can be done?
- Visit the dentist to confirm possible causes and to assess the severity.
- Different management approaches are necessary depending on the cause:
A. Stress management - it may help to talk to your child about any tension or fears before going to bed. Reading a favorite book or a warm bath may relax them as well.
B. Self care - many processed foods have additives that may contribute to “hyperactivity” .It may be a worthwhile exercise to cut down on such foods and assess the difference in behavior.
C. Dental approaches - Mouth guards may be made in some cases for the child to wear at night. In severe cases the dentist may suggest placing stainless steel crowns. Some children may be referred to other specialists if their jaws are a problem.
The good news is that most children do outgrow bruxism. The grinding gets less between 6-9 and actually stops between 9-12.
Treatment Options for Nursing Bottle Caries
- by Dr Geoffrey Melman BDS MSc(Dent)(Witwatersrand)
Speciality in Paediatric Dentistry (U.K.)

The premature loss or unsightly appearance of grossly decayed primary anterior teeth (nursing bottle caries) fig. 1 (“baby” or “milk” teeth) may physically handicap, embarrass and psychologically traumatise a young child.1,2,3,4 Left untreated, decayed teeth may cause pain and infection resulting in damage to the developing permanent tooth5 and feelings of personal inadequacy. 2, 3 Treatment of these badly decayed teeth will prevent pain and infection and assist the child to a better social and emotional adjustment.6,7
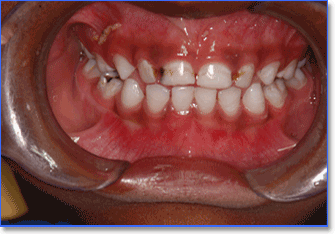
Fig. 1 - Nursing Bottle Caries
Treatment plans advocated for grossly decayed primary anterior teeth include extraction,8 partial dentures9,10 and restoration with various types of crowns e.g. Stainless Steel Crowns,7,11 Acrylic Jacket Crowns, Preformed Celluloid and Polycarbonate Crowns12 and chemically cured composite resins (tooth coloured filling material).4,13,14,15,16
Aetiology of Nursing Bottle Caries
Nursing bottle caries fig. 1 has derived its name from the uncontrolled use of the bottle fig. 2. The complex cause of nursing bottle caries has been fully covered in the article by Prof Sid Setzer on this web page.
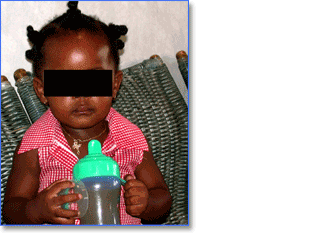
Fig. 2 - Child with nursing bottle filled with juice
Extraction of Decayed Teeth
The premature extraction of the diseased primary teeth is advocated only if the teeth are decayed beyond possible repair8 fig. 3. One should always bear in mind that the age of the patient is not an acceptable criterion in determining whether a primary tooth should be extracted. It should be noted that the loss of teeth can lead to numerous problems such as psychological trauma (children are very cruel towards each other),1,2,3,5,6,7 the inability to bite and chew food,5 developing tongue trusting and poor speech,1,5 loss of space with resulting orthodontic complications,2,7,17 tilting of adjacent teeth, the overeruption of the opposing teeth with resulting periodontal problems (gum disease),7 as well as the formation of fibrotic tissue (hard gums) which can retard the eruption of the permanent teeth.7
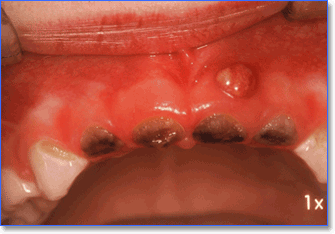
Fig. 3 - Grossly decayed primary anterior teeth with an abscess present
Partial Dentures
Partial dentures are a cost effective means of replacing lost or extracted teeth.1,2,7,9,10,18 Children readily adapt to the partial denture and find them comfortable to wear.10 fig. 4
A partial denture fig. 5 is advantageous in maintaining space,7 preventing the tilting of adjacent teeth,2,7 preventing the formation of fibrotic tissue7 encourages the eruption of the permanent teeth, does not interfere with the development of the upper jaw,7 provides normal dental function,2,7,19 maintains normal facial contours2,9 and aids in the attainment of normal speech patterns.2,7
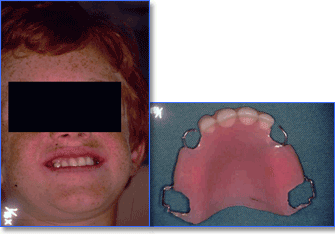
Fig. 4 - Child wearing partial denture as shown in Fig. 5
The major disadvantages of partial dentures are that they encourage plaque retention,5 which caused the original tooth decay; the partial denture is often lost at school and in the uncooperative child, the partial denture may not be worn.2
Crowns
The placement of crowns provides a very satisfactory means of restoring anterior teeth.4,11,13,15,16,20,21
Stainless Steel Crowns
These preformed crowns are routinely used to successfully restore posterior teeth fig. 6 and have been used to restore primary anterior teeth as well.7 However, they do not match the colour of the adjacent teeth and are therefore unsightly.11
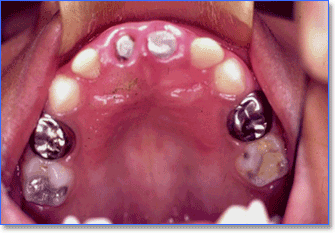
Fig. 6 - Stainless Steel Crowns on posterior teeth
Acrylic Jacket Crowns
Acrylic jacket crowns offer excellent aesthetics, are insoluble in oral fluids and resist surface staining.2,15 However, the material wears away rapidly, is expensive and the process requires long dental appointments.15
Composite Resin Crowns or "Strip Crowns"
Composite resin (tooth coloured filling material) can be successfully used for full coronal coverage to crown severely damaged primary teeth.4,13,14,15,16,20,21 These composite resin crowns look just like normal teeth fig. 7, wear well,16 prevent the development of a tongue thrust and bad speech habits, prevent the formation of fibrotic tissue with delayed permanent tooth eruption, prevent loss of space and the child cannot loose or fail to wear the crown.4,16 Composite resin can be polished to a smooth lustre thereby decreasing plaque accumulation. This cost effective treatment option does not require long dental appointments and lasts the life of the primary tooth4,16 and is thus the treatment of choice when restoring decayed primary anterior teeth.4,16
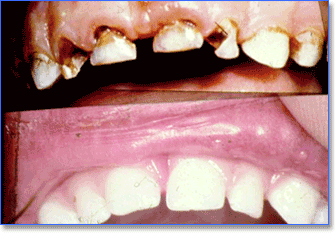
Fig. 7 - Nursing bottle caries of anterior primary teeth (top picture) restored with composite crowns (bottom picture)
References
- Cockburn, A. and MacGregor, A.R. (1961) Treatment of the edentulous child. The Dental Practitioner, 11,309-313.
- Rao, S.R. (1973) Removable partial dentures for children. In Clinical Paedodontics, Fourth Edition, Ed. Finn, S.B., Ch.12, Pages 271-285. Philadelphia: W.B. Saunders Company.
- Fisher, N.L. (1985) Restoration of anterior teeth: a transitional approach for the young adult. British Dental Journal, 158, 445-449.
- Rosen, M., Melman, G.E. and Cohen, J. (1990) Changes in a light-cured composite resin material to restore primary anterior teeth: an eighteen month in vivo study. Journal of the South African Dental Association, 45, 251-255.
- Joho, J and Marechaux, S.C. (1980) Prosthetic problem and solution in the primary dentition: report of a case. Journal of Dentistry for Children, 47, 50-52.
- Laird, W.R. (1970) Immediate dentures for children. Journal of Prosthetic Dentistry, 24, 358-361.
- Borjian, H. (1978) Removable prosthetics in pre-school children. Journal of Pedodontics, 2, 246-250.
- McCallum, C.A. (1973) Oral surgery for children. In Clinical Paedodontics, Fourth Ed. Finn, S.B., Ch. 18, Pages 391-393. Philadelphia: W.B. Saunders.
- Esposito, S. and Vergo, T.J. (1978) Removable overdentures in the oral rehabilitation of patients with dentinogenisis imperfecta. Journal of Pedodontics, 2, 304-315.
- Weintraub, S.G. and Yalisore, I.L. (1978) Prosthetic therapy for cleidocranial disostosis: report of a case. Journal of the American Dental Association, 96, 301-305.
- Croll, T.P. and Blum, J.R. (1982) The stainless steel crown for a primary canine tooth: a pictorial essay. Journal of Pedodontics, 6,301.
- Finn, S.B. and Ripa, L.W. (1973) Properties and uses of restorative materials. In Clinical Pedodontics Fourth Ed. Finn, S.B., Ch. 9, Pages 178-181. Philadelphia: W.B. Saunders.
- Webber, D.L. (1979) A method of restoring primary anterior teeth with the aid of a celluloid crown form and composite resins. Pediatric Dentistry, 1, 244-245.
- Croll, T.P. (1984) Dentin Adhesive Bonding: new applications (II). Quintessence International, 11, 1123-1129.
- Croll, T.P. (1985) Primary canine full coronal restorations: new considerations. Quintessence International, 2, 143-147.
- Melman, G.E. (1988) Changes in a light cured composite resin material used to restore primary anterior teeth: an eighteen month study. Research report submitted to the faculty of dentistry, University of the Witwatersrand, in part fulfilment of the requirements for the Degree of Master of Science in Dentistry.
- Wright, P. (1971) Partial dentures for children. New Zealand Society for Dentistry in Children Bulletin, 16, 4-5.
- Borjian, H. (1960) The effect of early dental treatment of anhydrolic ectodermal dysplasia. Journal of the American Dental Association, 61, 555-559.
- Kobren, A., Salvin, O. and Petrie, R.F. (1962) Partial denture prostheses for children. Dental Clinics of North America, 12, 761-777.
- Doyle, W.A. (1979) A new preparation for primary incisor jackets. Pediatric Dentistry, 1, 38.
- Rifkin, A.J. (1984) Acid-etch restorations in primary anterior teeth. Journal of the Dental Association of South Africa, 39, 385-387.
Children's Orthodontics
- by Dr. Anna-Paula de Freitas

Concerns of Parents and their growing children:
Signs or habits that may indicate the need for an early orthodontic examination: -
- Teeth that meet abnormally or not at all
- Jaws and teeth that are out of proportion to the rest of the face
- Crowding, misplaced teeth, missing teeth
- Mouth breathing
- Thumb sucking
- Difficulty chewing and biting
- Jaws that shift or make sounds
- Biting the cheek or roof of the mouth
- Early or late loss of teeth
Age for screening – 7 yrs
The American Association of Orthodontics recommends orthodontic screening no later than the age of seven. This enables the dentist to detect and evaluate problems (if any), advise if treatment will be necessary and a referral to an orthodontist. The best time for the patient to be treated can also be decided upon, growth related problems can also be identified at this time.
A child’s growth and orthodontic treatment can complement each other.
- A common problem is when the upper front teeth protrude (stick out in front) of the lower teeth. This may be because the incorrect inclination of these teeth. This may then be easily corrected by orthodontic therapy.
-
The lower jaw being shorter than the upper jaw:
- Orthodontic appliances can be used to help the growth of the lower jaw
- Abnormal swallowing may be eliminated
- Corrective surgery can be prevented at a later stage when there is slow jaw growth or none at all
- These appliances influence the jaw muscle to work in a way that improve forward development of the lower jaw. Some fixed some removable. You, your dentist and orthodontist can discuss which appliance is best for your child.
Can my child play sport while wearing braces?
Yes wearing a protective mouth guard is advised while playing sport. Your dentist or orthodontist can make a specific mouth guard. Not only does it protect the teeth but also acts as a shock absorber.
Can You Reverse Tooth Decay?
- by Dr. Stephan Horwitz (BDS(Wits))

Chewing sugar free gum for 20 minutes after meals and snacks has been shown to significantly reverse early signs of tooth decay.
Stimulated saliva contains a higher concentration of the same types of calcium, phosphate and hydroxyl ions that occur normally in teeth then unstimulated saliva,
Consequently, stimulated saliva is a more effective medium for remineralizing enamel crystals damaged by initial caries attack.
After meals and snacks, bacteria in plague produce acids, which cause the pH in the mouth to fall. If the pH falls below the critical level of 5.5 the tooth enamel starts to demineralize or dissolve and small white lesions may appear.
Stimulation of saliva flow results in an increase in the washing out of acids and also an increase in the amount and concentration of remineralization ions.
It is these ions that help to repair these early signs of tooth decay.
Remineralization of enamel lesions can occur with or without chewing sugar free gum. However, it has been shown that when patients chew sugar free gum regularly after meals and snacks remineralization is doubled in comparison with those who do not chew sugar free gum.
Stimulated saliva also has a higher concentration of bicarbonate, which raises the pH of saliva and greatly improves its buffering ability.
Stimulated saliva through chewing sugar free gum is therefore much more effective at neutralizing plague acids in the mouth.
Some sugar-free gums contain micro granules made of sodium polyphosphate-an ingredient proven to adhere to the surface of teeth to provide cleaning benefits such as stain prevention and removal, pellicle removal and prevention of calculus or tartar formation.
Another additive in some sugar free gums is xylotol, which is a naturally occurring non-fermentable polyol, which has been clinically proven to have anti-cariogenic properties in addition to helping reduce plague formation.
So,chewing sugar free gum stimulates saliva; helps clear food debris, neutralizes plague acid and remineralizes tooth enamel.
The chewing action also helps to remove surface plague.
Chewing sugar free gum should never replace brushing and flossing, but if it is used after eating or wherever brushing teeth is impractical it is an enjoyable way to help protect teeth from decay.











